Newborn Bloodspot Screening - Information for parents
This leaflet explains the conditions screened for and how the sample is taken.
This information is available in large print and Braille. Please ask your midwife or health visitor.
This animation gives you information on the bloodspot screening test that you will be offered for your baby once they are born. It shows how the test is taken and explains the conditions being screened for.
You will be offered a bloodspot screening test for your newborn baby for nine rare but serious conditions. The sample for this test is usually taken five days after your baby is born. This leaflet explains the conditions screened for and how the sample is taken. If you have any more questions, please talk to your midwife.
Contents
― Why should I have my baby screened?
― What are newborn babies screened for?
― Will screening for these conditions show up anything else?
― Who will take the bloodspot sample?
― How will the bloodspot sample be taken?
― Are repeat blood samples ever needed?
― Screening is recommended
― How will I hear about the results?
― What happens to your baby’s bloodspot screening card after screening?
― Using your information
Why should l have my baby screened?
-
Newborn bloodspot screening identifies babies who may have rare but serious conditions
-
Most babies screened will not have any of the conditions. However, for the small number that do, newborn bloodspot screening means that these babies can receive early specialist care and treatment
-
Early treatment can improve their health and prevent severe disability or even death
-
If a baby has a ‘suspected’ screening result for any of the conditions, they will need further tests to confirm that they have the condition
-
The test is safe and there is no known harm to your baby associated with having the test
What are newborn babies screened for?
In Wales all babies are offered screening for the following conditions:
- Inherited metabolic disorders:
- Medium-chain acyl-CoA dehydrogenase deficiency (MCADD)
- Phenylketonuria (PKU)
- Maple syrup urine disease (MSUD)
- Isovaleric acidaemia (IVA)
- Glutaric aciduria type 1 (GA1)
- Homocystinuria (HCU)
- Congenital hypothyroidism (CHT)
- Cystic fibrosis (CF)
- Sickle cell disorders (SCD)
Inherited metabolic disorders
Babies with these rare inherited disorders cannot process certain substances in their food. Without treatment, babies with these disorders will have serious long-term health problems and for some of the disorders babies can become suddenly and seriously ill.
Newborn screening means that babies who have one of these disorders can be identified early and have the right diet and treatment and specialist care to prevent health problems from developing.
It is very important to let your healthcare professional know if you have a family history of any of these metabolic disorders.
Babies are offered screening for the following six inherited metabolic disorders (IMDs):
-
Medium-chain acyl-CoA dehydrogenase deficiency (MCADD)
Babies with MCADD have problems breaking down fats to make energy for their body. If babies are not screened and have this disorder, the diagnosis may only be made when they become suddenly and seriously unwell. Three or four babies in Wales are born with MCADD each year.
-
Phenylketonuria (PKU)
Babies with PKU cannot break down an amino acid called phenylalanine. Amino acids are ‘building blocks’ of protein and we get protein from certain foods. If untreated, babies with PKU will develop
a serious permanent mental disability. Newborn screening means that babies can be identified and treated with a special diet to prevent this disability. Three or four babies in Wales are born with PKU each year.
-
Maple syrup urine disease (MSUD)
-
Isovaleric acidaemia (IVA)
-
Glutaric aciduria type 1 (GA1)
-
Homocystinuria (HCU)
Babies with MSUD, IVA, GA1 or HCU cannot break down certain amino acids that are contained in the protein we eat, in the usual way. This leads to harmful levels of certain amino acids and other harmful chemicals in the blood. These are rare disorders and it is expected that one or two babies in Wales will be born with one of these disorders each year.
Congenital hypothyroidism (CHT)
Babies with congenital hypothyroidism do not
have enough of the hormone thyroxine. Without this hormone, they do not grow properly and can develop a serious, permanent, physical and mental disability.
Approximately 18 babies in Wales are born with CHT each year.
Newborn bloodspot screening means that babies with CHT can be identified and treated early with thyroxine tablets. This treatment will prevent serious disability and allow the baby to develop normally. If babies are not screened and are later found to have CHT, it may be too late to prevent them becoming seriously disabled.
Cystic fibrosis (CF)
This inherited condition affects digestion and the ability of the lungs to work properly. Babies with CF have problems digesting food and may not gain weight well. They are also more likely to have frequent chest infections.
Between 12 and 14 babies in Wales are born with CF each year.
Newborn bloodspot screening means that babies with CF can be identified and treated early with a high-energy diet, medicines and physiotherapy. Early treatment is thought to help children with CF live longer, healthier lives. If babies are not screened for CF and they do have the condition, they can be tested later, but parents may have an anxious and uncertain time before CF is diagnosed.
Sickle cell disorders (SCD)
These are inherited disorders that affect the red blood cells. If a baby has a sickle cell disorder,
their red blood cells can change to a sickle shape and become stuck in the small blood vessels. This causes pain and damage to the baby’s body, serious infection, or even death.
Three or four babies in Wales are born with a sickle cell disorder each year.
Newborn bloodspot screening means that babies with SCD can be identified, and receive early treatment, including immunisations and antibiotics. This, along with information and support for parents, will help prevent serious illness and allow the child to live a longer and healthier life.
Will screening for these conditions show up anything else?
Occasionally, other medical conditions might be identified through these screening tests. Screening may identify babies who are genetic carriers of the conditions tested or of other unusual red blood-cell disorders.
Screening for cystic fibrosis (CF) includes testing some babies for the most common gene changes that cause CF. This means screening may identify some babies who are likely to be genetic carriers of CF. These babies may need further testing to find out if they are a healthy carrier or have CF. Carriers of CF are healthy, and will not be affected by the disease.
Who will take the bloodspot sample?
Newborn bloodspot screening is carried out five days after your baby’s birth. Occasionally this may be later than five days. The sample is usually taken by the midwife in your home, or in the hospital.
Other health professionals, who have been trained to carry out newborn bloodspot screening, may take the sample.
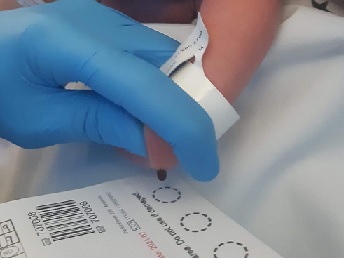
How will the bloodspot sample be taken?
The midwife will prick your baby’s heel using a special device to collect four drops of blood onto a newborn bloodspot screening card. Collecting these bloodspots usually takes a few minutes. The card is sent to the Newborn Screening Laboratory in Cardiff for testing. The midwife will write your baby’s details on the card to identify them.
The heel prick may be uncomfortable and your baby may cry.
You can help by:
- making sure your baby is warm and comfortable, and
- cuddling your baby and giving them a feed.
Are repeat blood samples ever needed?
Occasionally the midwife or health visitor will contact you and ask to take a second blood sample from your baby’s heel.
This may be because:
- there was not enough blood collected
- the information recorded on the bloodspot card was incomplete
- the result was unclear
- your baby was born early, or
- your baby had a blood transfusion before the test.
Your midwife or health visitor will explain the reason to you. It is important that if a repeat test is needed it is done promptly so that all the tests have been completed within the early weeks of life.
Screening is recommended
Screening your baby for all the conditions discussed is recommended by the NHS.
The midwife will make sure that you have the opportunity to ask any questions that you have after reading this leaflet, and at least 24 hours before the sample is taken.
Before taking the bloodspot sample, the midwife will provide another opportunity to discuss the screening, and answer any questions you may have. You will be asked for your consent (permission) for your baby to have newborn bloodspot screening.
If you do not want your baby screened for any or all of these conditions, please let your midwife know. Please note that screening for the six inherited metabolic disorders is carried out as one test. This means that it is not possible to have your baby screened for only some of the inherited metabolic disorders.
The midwife will record any conditions you don’t want screening for on your baby’s newborn bloodspot screening card. You will be asked to sign the screening card to confirm this. Your GP and health visitor will be told.
If you change your mind and want your baby to have newborn bloodspot screening in the future, please let your health visitor know. They will make arrangements for this to be carried out. Newborn bloodspot screening is offered to all babies up to one year of age. However, screening for cystic fibrosis is only offered up to eight weeks of age because the test becomes unreliable after this time.
All your decisions will be recorded in your maternity record and in your baby’s personal child health record (often referred to as their ‘red book’).
If you have any concerns about your baby’s screening, please discuss them with your midwife, health visitor or GP.
How will I hear about the results?
Most babies will have ‘not suspected’ results, which mean that they probably do not have any of the conditions screened for. These results will be sent to you in a letter within six weeks of the sample being taken. Your health visitor will discuss the results with you and answer any questions you may have.
If your baby’s screening result shows that they may have congenital hypothyroidism or an inherited metabolic disorder, you will usually be contacted in person or by phone before your baby is three weeks old. You will be told about the tests that will be needed to make the diagnosis. You will also be given an appointment to see a specialist.
If your baby’s screening result shows that they may have cystic fibrosis, you will usually be contacted in person before your baby is four weeks old. You will be told about the tests that will be needed to make the diagnosis, and will be given an appointment to see a specialist.
If your baby is thought to have a sickle cell disorder you will usually be contacted before your baby is six weeks old. You will be told about the tests that will be needed to make the diagnosis, and will be given an appointment to see a specialist.
The timing for receiving the screening results given above relies on the newborn bloodspot screening tests being carried out five days after birth.
If you move home while you are waiting for the results of your baby’s screening test, please tell your midwife or health visitor your new address.
The purpose of screening is to identify babies more likely to have these conditions.
Screening is not 100% accurate.
- Sometimes, a baby with a ‘suspected’ screening result may, after having further tests, be found not to be affected by the condition.
- In other cases, a baby with a ‘not suspected’ screening result may later be found to have the condition. This only happens rarely.
What happens to your baby’s bloodspot screening card after screening?
After screening, the section of the bloodspot card that has the written details of your baby is separated and destroyed. The section with the bloodspots is identified by a barcode number unique to both the card and your baby. This section will be stored securely for at least five years and may be used:
- to check the result
- to carry out other tests recommended by your doctor
- to improve the screening programme, or
- for research to help improve the health of babies and their families in the UK.
This research will not identify your baby, and you will not be contacted. There are strict laws that govern the use of the bloodspots and legally we have to keep to these.
In the future, researchers may want to invite you or your child to take part in research that has been agreed by the Screening Division of Public Health Wales. This will only be for research projects that have been approved by a Medical Research Ethics Committee and the researchers will need to get your permission to be involved. If you do not want to be invited to take part in research, please let your midwife know and this information will be recorded on the bloodspot card.
Using your information
For us to contact you as part of the programme, we will need to handle some of your and your baby’s personal information. If you need more information about this, you can:
- read our Privacy Notice
- email: PHW.InformationGovernance@wales.nhs.uk, or
- phone: 029 2010 4307.
We also keep personal details to make sure that the standard of our service is as high as possible. This includes checking your baby’s records if your baby is found to have a condition after having a screening test which showed a ‘not suspected’ result.
We only ever publish information as statistics and we never publish personal details. We pass on your personal information to health professionals or organisations that need it, including your GP, health visitor and consultant paediatrician. These professionals must protect the personal information in the same way as we do.
All our paper and computer records are stored and processed securely, away from public access.
If you would like to tell us about your experience of newborn bloodspot screening, please click here.